Country-to-Country Visits
Featured Visits: 2023
Eswatini, Nigeria Rwanda
From July 10 to 14, 2023, Rwanda hosted the first CQUIN-supported enhanced learning visit for a 14-member delegation, including members of the Nigeria and Eswatini Ministries of Health and National Networks of People Living with HIV. The visit aimed to foster discussions, identify best practices, and co-create resources to support the integration of family planning (FP) and HIV programs.


Sierra Leone Uganda
From June 19 to 24, 2023, CQUIN supported a learning visit for a delegation from Sierra Leone to Uganda. The Sierra Leone delegation, which included the HIV Program Manager, the Monitoring and Evaluation (M&E) Coordinator, the Senior Health Products Manager, the DSD Advisor, and the Executive Director of the Network of HIV Positives in Sierra Leone, learned about Uganda’s experience in implementing community-based and facility-based antiretroviral therapy (ART) models, from Uganda’s policies to the M&E of DSD and viral load utilization.
South Africa Nigeria
From February 19 to 24, 2023, the Nigeria Ministry of Health, led by Irene Esu, MBBS, MPH, FMCPH, ART coordinator, hosted a five-day learning visit for a delegation from South Africa. The visit included trips to a primary health care facilities, a major district hospital, and three community pharmacies.

Featured Visits: 2022

Tanzania Nigeria
Tanzania aims to further improve the quality and coverage of HIV treatment services by introducing a new differentiated service delivery model: community ART dispensing. To help develop a roadmap for this new goal, the Tanzania Ministry of Health and Social Welfare requested CQUIN support for a country-to-country visit to Nigeria to learn about their decentralized community pharmacy model.
Eswatini, Mozambique, Zambia Tanzania
From March 29 to April 1, 2022, the Tanzania Ministry of Health and Social Welfare (MOH) National AIDS Control Program hosted the three country teams. Visitors learned how Tanzania designs its key and vulnerable populations (KVP) programs, specifically methadone-assisted therapy (MAT) clinics for people who inject drugs and community services for key populations.


Ethiopia Eswatini
Since the CQUIN workshop for AHD in July 2020, Ethiopia has prioritized the launch of a DSD model for AHD. From February 1 to February 5, 2022, CQUIN supported a country-to-country learning exchange that allowed Ethiopia to see how AHD could be coordinated, implemented, and monitored.
Featured Visits: 2021
Kenya Nigeria
The Kenya National AIDS/STI Control Program (NASCOP) visited Nigeria from December 6-10, 2021 for a CQUIN south-to-south exchange to learn about Nigeria’s community pharmacy and 6-MMD models.
During the visit, the Kenya team learned about Nigeria’s implementation of 6-MMD including policy guidance, procurement, supply chain and buffer stocks, facility and community management of ART stocks and medication, and engaging recipients of care in the model. Nigeria also presented the successes and challenges of implementing decentralized ART distribution through private pharmacies, and the monitoring and evaluation (M&E) of systems set up to support both 6-MMD and decentralized ART distribution through private pharmacies.


Burundi Côte d’Ivoire
CQUIN supported three members from the Burundi Ministry of Health’s National Program for the Fight Against AIDS and Sexually Transmitted Infections (PNLS) and a member of Burundi’s Association Nationale de Soutien aux Séropositifs et Malades du SIDA (ANSS, the national network of people living with HIV) to visit Côte d’Ivoire in a learning exchange.

Liberia Nigeria
From September 13 to 18, 2021, CQUIN supported a delegation from Liberia’s National AIDS and STI Control Program (NASCP) to Nigeria for a south-to-south learning exchange. The trip was also an opportunity for the Liberian delegation to observe Nigeria’s approach to monitoring and evaluation (M&E) of DSD models.
Côte d’Ivoire Eswatini
Eswatini’s Ministry of Health hosted representatives from Côte d’Ivoire for a CQUIN-supported south-to-south learning exchange from May 11 to May 16, 2021.
The Eswatini country team organized visits to three health facilities where the Côte d’Ivoire team learned about the Eswatini approach to DSD implementation for people with advanced HIV disease (AHD).


Senegal Côte d’Ivoire
Representatives from Senegal visited Côte d’Ivoire in the first CQUIN supported south-to-south learning exchange since the COVID-19 pandemic halted travel last year.
Côte d’Ivoire’s Programme National de Lutte Contre le Sida (National Program to Fight HIV/AIDS or PNLS) hosted the three-person Senegalese delegation, which included the Ministry of Health focal person for care and treatment, the Ministry of Health focal person for monitoring and evaluation, and the national representative for people living with HIV.
Featured Visits: 2020

Liberia and Uganda Ethiopia
Delegates from the Liberia and Uganda National HIV/AIDS Control Programs, Central Medical Stores, and national networks of people living with HIV traveled to Ethiopia to learn how the Ministry of Health (MOH), and implementing partners planned and scaled up the appointment spacing model (ASM) and six multi-month dispensing (6-MMD).
The trip was hosted by the Ethiopian MOH and led by ICAP’s CQUIN project. MOH representatives updated the two visiting delegations on national strategy and DSD implementation in the country, with a particular focus on ASM. The visiting teams also had the opportunity to provide constructive feedback on Ethiopia’s community ART refill group (CARG) model.

Côte d’Ivoire and Ethiopia Zimbabwe
In February 2020, delegates from Côte d’Ivoire and Ethiopia’s Ministries of Health (MOH), National AIDS Program staff, and civil society representatives traveled to Zimbabwe to observe the implementation of community and facility-based DSD models.
The visit, hosted by the Zimbabwe Ministry of Health and Child Care (MOHCC) and coordinated by ICAP’s CQUIN project, was an opportunity for the Ivorian and Ethiopian delegations to observe the implementation of Community ART Refill Groups (CARGS) and facility-based models like Fast Track in urban and rural settings.
Featured Visits: 2019
Mozambique and Eswatini Ethiopia
In October 2019, delegates from the Mozambique National HIV/AIDS Program and the Eswatini National AIDS Program traveled to Ethiopia to learn how Ethiopia’s Federal Ministry of Health (FMOH) and implementing partners are using the appointment spacing model (ASM)—a method of spacing clinical visits and medication refills every 6 months—to administer antiretroviral therapy (ART) and improve the scale-up of DSD.
The visit provided a unique opportunity for the group to observe the procurement, storage and distribution processes for medication, as well as learn how this model has led to improved service delivery in Ethiopia.
READ MORE
Alongside FMOH, the group met with the Ethiopia Pharmaceutical Supply Agency and a recipient of care group to delve into the details of supply chain, gaining an understanding of how the functionality of facility-level services impact recipients of care.
The Ethiopia team explained that at the national level, the MOH identified an ART focal person and formed a multi-disciplinary expert panel/technical working group to monitor and support the implementation of ASM. Training materials, SOPs, job aides, and data capturing and reporting tools were developed with support from ICAP Ethiopia. With support from EPSA and Central and Regional Health Bureaus, Ethiopia MOH conducted a baseline health facility assessment for pilot sites and identified gaps and challenges for ASM implementation.
The Ethiopia team highlighted ASM implementation challenges including antiretroviral therapy (ART) stock hoarding by some facilities for fear of stock outs; an unexpectedly high rate of refusal of ASM by recipients of care attributed to concerns about privacy and stigma; and a parallel reporting system for ASM leading to suboptimal timeliness and completeness of data reporting. Recommendations for successful implementation of ASM were for countries to adopt 90-tablet ART containers to reduce the load of ARVs carried by recipients of care; integrating ASM reporting into monthly national health information reporting system to avoid parallel reporting; adding supportive supervision of ASM in clinical mentoring visits, and planning for comprehensive evaluation of ASM implementation in advance.
The visiting teams from Eswatini and Mozambique found the trip to be useful and informative and gained confidence in their respective countries’ ability to implement the model. They learned that leadership, commitment, community engagement for demand creation, regular supportive supervision, strong collaboration between the program and the logistics management unit and regular coordination meetings are key to the successful implementation of ASM.
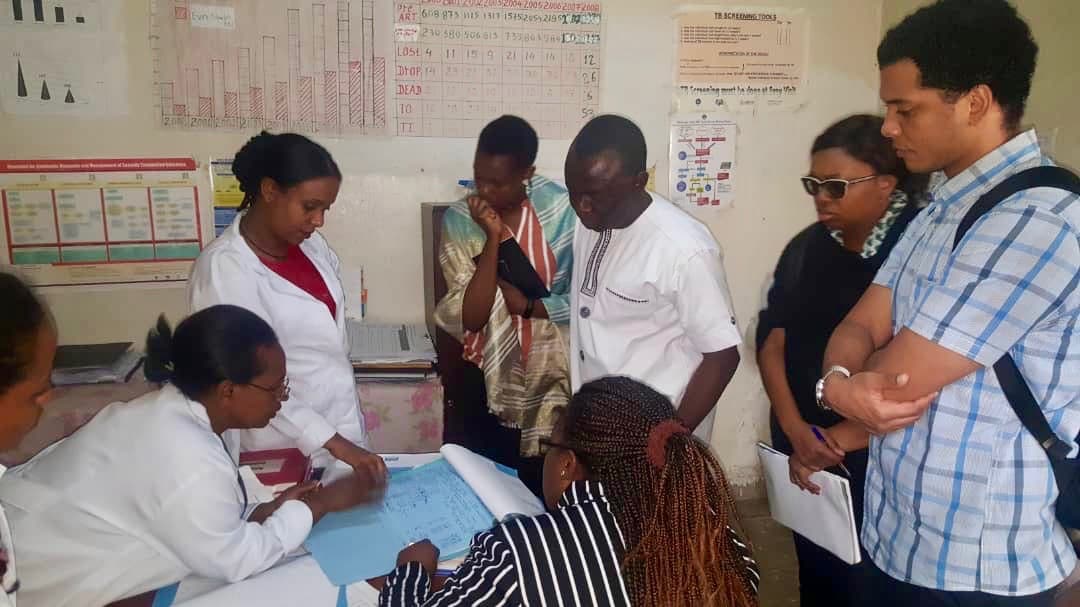
Tanzania and Zambia Uganda
In April 2019, representatives from Tanzania’s National AIDS Control Program (NACP), the National Council of People Living with HIV in Tanzania (NACOPHA), and the Centers for Disease Control and Prevention in Tanzania alongside representatives from Zambia’s Ministry of Health visited Uganda to observe more-intensive DSD models, and to understand the coordination process between facility and community-level DSD planning, implementation and monitoring.
Uganda’s Ministry of Health hosted the visit and provided the group with a country-level update on DSD implementation. Additionally, The AIDS Support Organization (TASO), a pioneer in Uganda’s HIV/AIDS response, facilitated a visit to a Community Drug Distribution Point (CDDP), Community Client-Led ART Delivery (CCLAD) and facility-based DSD models.
READ MORE
The group also visited a district hospital, supported by Makerere University and observed implementation of the facility-based individual model (FBIM); fast-track drug refills; and facility based treatment groups including teen clubs. The team was further hosted by Infectious Disease Institute (IDI) outreach team, to observe their Community Pharmacy drug Refill Program.
A CDDP consists of a number of CCLAD groups, each of which has 10 or fewer clients who meet quarterly to collect their drugs at a designated area. The CCLAD are self -formed groups, with one group leader appointed by the group members. The leaders are trained to screen for TB; measure and interpret weight and mid-upper arm circumference (MUAC); assess ART adherence via pill counting; screen for gender-based violence (GBV) and sexually transmitted infection; distribute condoms, and provide health education. The CCLAD leaders also provide health education and promote HIV testing to community members, helping to combat stigma and identify people who are HIV positive at the community level.
The community pharmacy drug refill model uses selected private pharmacies within the city to serve as drug pick up points for people doing well on ART. The visiting teams from Tanzania and Zambia had the opportunity to observe drug refills at two community refill pharmacies, review the tools used for drug refills, and discuss the model with the pharmacy nurse in charge of the program.
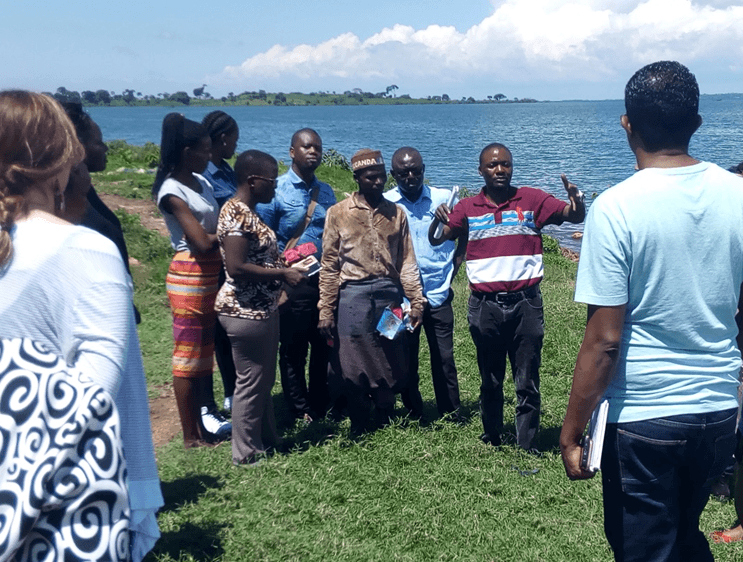
Featured Visits: 2018

Eswatini, Kenya, and Malawi Uganda
In June 2018, teams from Eswatini, Kenya, and Malawi visited Uganda on a joint south-to-south learning exchange hosted by the Uganda Ministry of Health National AIDS Control Program. The teams also visited The AIDS Support Organization (TASO). The exchange included two field visits to observe CDDP and CCLAD models in action.
The visiting teams learned about the implementation of facility- and community-based DSD models for people living with HIV in urban and rural settings; community engagement and demand creation; and how community-based ART service delivery data flows into the national monitoring and evaluation system. Each team identified challenges and opportunities to adopt or adapt TASO’s DSD models for use by their country’s DSD program.
Zambia Eswatini
In June 2018, a team from Zambia’s Ministry of Health visited Eswatini on a joint south-to-south learning exchange hosted by the Eswatini National AIDS Program (ENAP) and ICAP Eswatini. The team visited two hospitals in Mbabane to learn about community-based integrated ART outreach and to observe early-morning refill models. The visit provided a unique opportunity for participants to see the implementation of client-centered services firsthand at the facility and community levels. In addition, the team attended a facility-based demonstration of Eswatini’s existing Client Management Information System (CMIS), where they observed how the system is used to manage patients on ART and link to other health conditions in addition to HIV.
Following the visit, Zambia’s Ministry of Health integrated the early morning refill model into their National DSD Guidelines, and an early morning clinic was launched at the University Teaching Hospital (UTH) in Zambia, providing new and diversified options for ART refills for recipients of HIV care in Zambia.


Zimbabwe South Africa
In November 2018, Ministry of Health staff and representatives of national networks of people living with HIV from Zimbabwe visited the Centre of AIDS Programme of Research in South Africa (CAPRISA) to observe more-intensive DSD models. Visitors observed CAPRISA’s best practices regarding management of patients with unsuppressed viral load and the Advanced Clinical Care program in KwaZulu-Natal. Lessons learned included ways to identify recipients of care due for viral load testing, the use of a dedicated “viral load failure” clinic model, and the delivery of enhanced adherence counseling.
Following the visit, representatives from Zimbabwe developed goals to include viral load performance when measuring DSD implementation success, and to increase viral load coverage by holding stakeholder and community engagement sessions.
Featured Visits: 2017
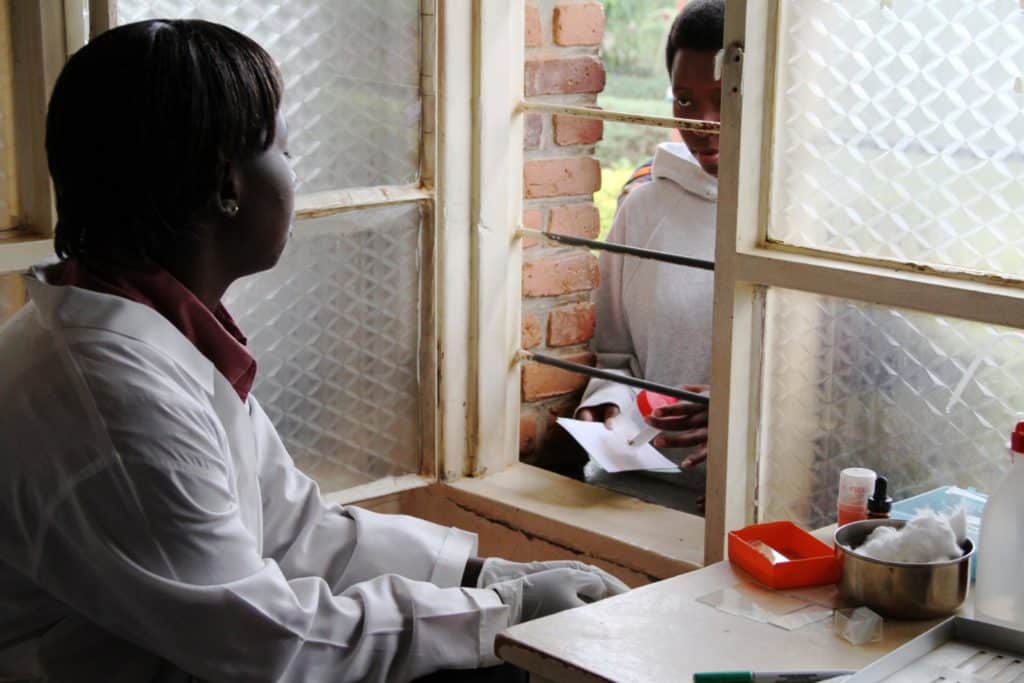
Mozambique Eswatini
In August 2017, a team from Mozambique’s Ministry of Health visited Eswatini to learn more about the implementation of DSD. They observed how Eswatini’s Ministry of Health planned, implemented, and sustained after-hours ART refills as well as their outreach model, where a health facility team pays monthly visits to a rural community.
Following the visit, Mozambique has successfully piloted the after-hours ART refill model in one facility, providing an alternative method for recipients of care to receive medication.

Eswatini Malawi
In June 2017, Eswatini’s Ministry of Health observed that Malawi had successfully integrated antiretroviral therapy (ART) refills and viral load monitoring into their teen clubs.
Representatives from the Eswatini National AIDS Program (ENAP) visited Malawi in May 2017 to learn about best practices related to DSD for adolescents living with HIV and the success of their teen club model. At that time, more than 9,300 adolescents living with HIV had been enrolled in 135 teen clubs located in 26 of Malawi’s 28 districts.
Eswatini translated these lessons into action by including the Malawi approach in their 2017 HIV Integrated Management Guidelines. Eswatini is now working to upgrade all teen clubs in the country to Treatment Clubs and has developed guidance on transitioning of adolescents to adult HIV treatment systems. In addition, relevant indicators for the treatment clubs have been added to the National Client Management Information System (CMIS) DSD module.

